Ava Publishes Peer-Reviewed Clinical Paper
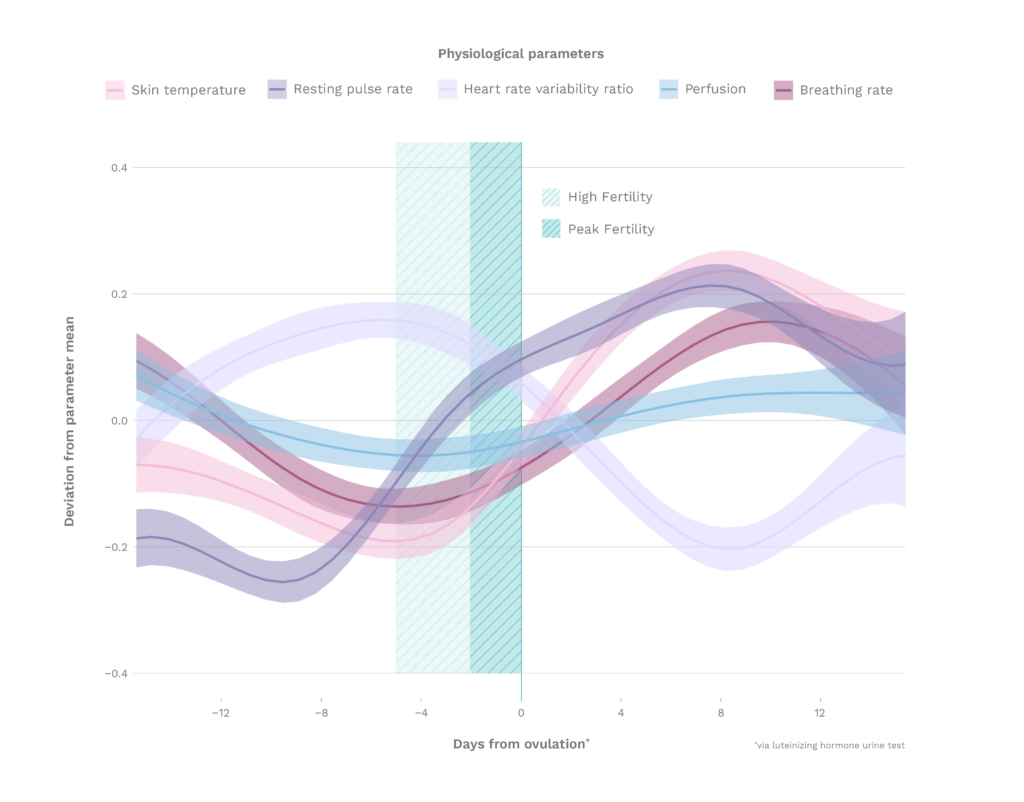
When it comes to female reproductive health—and specifically, the menstrual cycle—there’s a dearth of research and scientific understanding. Ava is proud to announce the publication of a peer-reviewed clinical paper that sheds unprecedented light on this issue.
This study sought to understand what phase-based differences (meaning, physical changes across different phases of the menstrual cycle) a wearable bracelet could detect in users’ wrist-skin temperature, heart rate, HRV, respiratory rate, and skin perfusion. Using insights from artificial intelligence and machine learning, the study then examined whether an algorithm could accurately identify the fertile window in real-time.
What we wanted to see from this study is if wearable sensor technology could help women track physiological changes across their menstrual cycles, and whether this method could fill the present gap between expensive ovulation detection (like sonograms) and free, less-precise fertile window approximation (like traditional BBT measurements).
This study represents the first of its kind to research multiple physiological changes concurrently across the menstrual cycle. And drawing on insight from artificial intelligence and machine learning, the study revealed that the Ava algorithm could detect the 5 most fertile days in real-time.
Phases of the menstrual cycle
In keeping with previous research, we divided the menstrual cycle into the following 5 phases:
- menstruation, starting with the first day of the period and lasting 5 days
- the follicular phase, starting on the first-day post menses and lasting through 6 days before ovulation (OV –6)
- the fertile window, starting 5 days before ovulation and lasting through ovulation (OV –5 to OV)
- the early luteal phase, starting 1 day after ovulation through a week after ovulation (OV+1 to OV+7)
- the late luteal phase, starting 8 days after ovulation (OV+8) and lasting through the day before the onset of menses
Study set up
To conduct this prospective longitudinal study, we recruited 237 conception-seeking Swiss women. All participants wore the Ava bracelet nightly while sleeping. They continued in the study for up to a year—or until they became pregnant. In addition to syncing the device to the Ava app daily, women also recorded their activities in the past 24 hours. Finally, women took a urinary luteinizing hormone test at several points in a given cycle to determine the close of the fertile window. The study showed that there were changes in physiological signals during different phases of the menstrual cycle and then trained a machine learning algorithm to recognize the fertile window.
After analyzing the clinical data, we observed significant changes in physiological signals, as captured by the wearable device across the menstrual cycle. Changes in the following physical signs were found:
- Wrist Skin Temperature
- Heart Rate
- Heart Rate Variability
- Respiratory Rate
- Skin Perfusion
What do these findings mean in a broader sense?
What is so exciting about this paper is that it reveals an important truth about the menstrual cycle: temperature is not the only thing that changes during the different phases of the cycle. In fact, we see changes in 5 different signals throughout the cycle, and by tracking those parameters simultaneously, we can detect when a woman is fertile. Until now, what was understood about the menstrual cycle was that only 1 signal—temperature—that changed.
But we found that 4 other physiological signals also change and that tracking all 5 of these signals together allows us to detect the fertile window in real time. No other product tracks all 5 of these signals. We are proud to publish these findings in a peer-reviewed journal, both because it proves that Ava’s novel, multi-parameter fertility tracking algorithm is capable of detecting the fertile window with 89% accuracy (confidence interval 0.89 – 0.92) and because it expands scientific understanding of women’s health.
Why is Ava publishing this study?
Ava’s vision as a company is that we become a long-term companion for women, giving them scientific and data-driven insights across all stages of their reproductive lives. We aim to do so through clinical research and Artificial Intelligence. In the past, medical researchers have thought of women’s bodies as unruly, complicated, or mysterious—and this is part of the reason why we still don’t fully understand menstrual hormones and how they impact women’s health.
Our vision is a big part of why we published our paper. And in publishing, not only have we gotten the proof that our algorithm works, but we have also improved the understanding of women’s bodies for all.











